Eye Doctors Work To Treat Glaucoma In Long Beach
August 28, 2017
Dr. Julia Song (left) with Christine C. talking about glaucoma impacts.
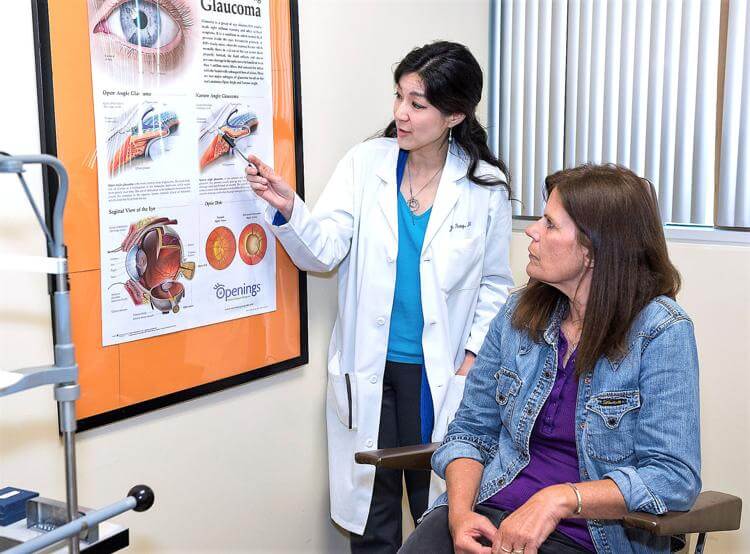
Blurry vision forced Christine C. to focus on her health.
The Long Beach resident said she knew that regular eye exams were important, but she hadn’t scheduled one in a while. Her eyesight scare spurred her to immediate action.
Christine’s mother lost her vision to glaucoma and Christine said she was afraid of a similar outcome, since family history greatly increases the chance of contracting the disease. Unwilling to wait six months for an ophthalmology appointment through her insurance company, Christine searched for a better solution and found EyeCare America. For the past 30 years, this organization has teamed with volunteer ophthalmologists to provide eligible patients with no-cost eye exams.
Twin doctors Julia and Alice Song share a practice with offices in Long Beach, Los Alamitos and Pasadena. The two say they are staunch believers in outreach; yearly medical mission trips have taken them to Mongolia, Mexico, Thailand, North Korea and the Philippines. Ten years ago, EyeCare America asked the Songs to offer free exams to eligible U.S. patients. They agreed.
“If you find and treat eye diseases before they become more advanced,” Dr. Alice Song said, “the outcome is better for the patient and for society. Some people become disabled from problems that could have been prevented by regular exams.”
EyeCare America sent Christine to see Dr. Julia Song. Song identified narrow angle glaucoma, a form of the disease that can be remedied through laser treatment. Song suggested surgery and provided the paperwork Christine would need. Christine’s insurance company authorized her for surgery, correcting the problem. Christine’s vision is now fine.
“My mom’s vision loss was frightening… I can’t even imagine,” Christine said. “I felt very grateful to have assistance from EyeCare America. They had a questionnaire, so I filled out the info and I fit the criteria. Then they sent me something in the mail setting up my appointment with Dr. Song. She was great.”
Christine said that glaucoma doesn’t give warning signs, it just attacks. At that point, she said, it’s usually too late.
“My blurred vision wasn’t related to glaucoma, but it got me to make the appointment,” she said. “I had the surgery done and now I’m good.”
The Songs said the number of EyeCare America patients they see has fluctuated over the years, ranging from six to 60 referrals per year. They said they are happy to see EyeCare America patients and they hope more people find out about the helpful program.
“If we catch problems early enough,” Dr. Julia Song said, “there are ways to help people. Christine C. was worried about her family history; her exam identified a problem and a solution. Our job as health care professionals is to help people find their way.”
The Song sisters haven’t limited their care to humans. Over the years, they have treated the eyes of some of their patients’ pets and even adopted a blind puppy. The two women said they couldn’t resist “Pappy,” who is part Papillion, after seeing him at a shelter two years ago. Although they said they couldn’t restore his sight, they put bubble wrap around the obstacles in their home and made him part of the family. Outreach seems to be integral to the doctors’ DNA.
To learn more about EyeCare America, go to www.aao.org/eyecare-america.
Original article, click here.
Selective laser trabeculoplasty success in pediatric patients with glaucoma: two case reports
August 15, 2013
Selective laser trabeculoplasty success in pediatric patients with glaucoma: two case reports.
Song J, Song A, Palmares T, Song M
J Med Case Rep. 2013 Jul 26;7(1):198. doi: 10.1186/1752-1947-7-198. PMID: 23889862 [PubMed] Free Article
Source
Long Beach Memorial Medical Center, 2840 Long Beach Boulevard, #330, Long Beach, CA 90806, USA. [email protected].
Abstract
INTRODUCTION:
Selective laser trabeculoplasty is a treatment option to lower intraocular pressure in patients with glaucoma. It has been proven to work in adults. We describe two pediatric patients with glaucoma who responded well to selective laser trabeculoplasty.
CASE PRESENTATIONS:
Two patients with pediatric glaucoma underwent selective laser trabeculoplasty. Patient 1 was a nine-year-old Iranian Asian girl with secondary aphakic glaucoma who was taking four glaucoma medications. She had a 50% decrease in intraocular pressure five weeks after selective laser trabeculoplasty. She was able to discontinue all four glaucoma drops after treatment. Patient 2 was a 13-year-old Filipino Caucasian boy who presented with early juvenile open-angle glaucoma and who was on no medications. He had a 40% drop in intraocular pressure four weeks after selective laser trabeculoplasty.
CONCLUSION:
Selective laser trabeculoplasty can decrease intraocular pressure in pediatric patients with glaucoma, both as a primary and secondary therapy. This study demonstrates that selective laser trabeculoplasty is a good option for the treatment of glaucoma in the pediatric population.
Repositioning of glaucoma tubes into the pars plana for refractory malignant glaucoma: a case report
August 15, 2013
Song J, Castellarin A, Song M, Song A.
J Med Case Rep. 2013 Apr 11;7(1):102. doi: 10.1186/1752-1947-7-102.
PMID: 23577950 [PubMed] Free PMC Article
Song J, Castellarin A Song M, Song A
Source
Long Beach Memorial Medical Center, 2840 Long Beach Blvd, , #330, Long Beach, CA 90806, USA. [email protected].
Abstract
INTRODUCTION:
Malignant glaucoma occurs when the intraocular pressure elevates in the setting of a shallow anterior chamber and patent iridectomy. We describe a case in which malignant glaucoma that was refractory to conventional treatment and complete vitrectomy was successfully managed by rerouting the glaucoma tubes into the pars plana.
CASE PRESENTATIONS:
A 47-year-old Latino man had a history of neovascular glaucoma and subsequent peripheral anterior synechiae. He was status post-two glaucoma drainage devices. He developed pupillary block. Laser iridotomy was performed without complications. He subsequently developed malignant glaucoma that was refractory to yttrium aluminum garnet capsulohyaloidotomy of the anterior hyaloid. He underwent pars plana vitrectomy with successful control of his intraocular pressure. After 2 weeks, the malignant glaucoma recurred. He underwent repositioning of the tubes into the pars plana with successful control of his intraocular pressure.
CONCLUSION:
In rare cases of malignant glaucoma refractive to yttrium aluminum garnet hyaloidotomy and vitrectomy, placement of glaucoma drainage devices is a reasonable alternative.
Sebaceous cell carcinoma of the ocular adnexa: clinical presentations, histopathology, and outcomes
August 15, 2013
Sebaceous cell carcinoma of the ocular adnexa: clinical presentations, histopathology, and outcomes.
Song A, Carter KD Syed NA, Song J Nerad JA
Ophthal Plast Reconstr Surg. 2008 May-Jun;24(3):194-200. doi:
10.1097/IOP.0b013e31816d925f.
PMID: 18520834 [PubMed - indexed for MEDLINE]
Source
Department of Ophthalmology and Visual Sciences, Carver College of Medicine, University of Iowa Hospitals and Clinics, Iowa City, Iowa, USA.
Abstract
PURPOSE:
To investigate the clinical features, time to diagnosis, histopathology, treatment, and mortality rates of patients with sebaceous cell carcinoma.
METHODS:
This was a retrospective, consecutive series of patients with sebaceous cell carcinoma at a tertiary referral medical center. Between January 1984 and January 2006, 31 patients with sebaceous cell carcinoma were evaluated at the Department of Ophthalmology and Visual Sciences, University of Iowa Hospitals and Clinics. The main outcome measures were clinical presentations, treatments, reconstructive procedures, and outcomes.
RESULTS:
Thirty-one patients were diagnosed with sebaceous cell carcinoma of the ocular adnexa on histopathology. Twenty (65%) of the patients were women and 11 were men. The upper eyelid was involved in 18 patients, lower eyelid in 10, both upper and lower eyelids in 1, and caruncle in 2. Twenty-three patients had in situ disease, pagetoid disease, or both. Eight patients reported symptoms for less than 6 months and 22 had symptoms for greater than or = 12 months before the diagnosis of sebaceous cell carcinoma was made. Local surgical excision of the tumor as initial treatment was performed in 25 patients. Exenteration was the initial surgery performed in 4 patients. Two patients died from metastatic sebaceous cell carcinoma.
CONCLUSIONS:
Sebaceous cell carcinoma has varied presentations and is commonly misdiagnosed. Tumor-related deaths occurred in only 2 patients (6.7%), which is lower than previous reports and may be related to earlier detection or improved surgical excision techniques.
Intraocular pressure improvement in patients receiving teprotumumab for the treatment of thyroid eye disease: a case series
May 10, 2022
J Med Case Rep. 2022 May 10;16(1):195. doi: 10.1186/s13256-022-03375-x.
Abstract
Background:
Teprotumumab is a novel treatment that reduces inflammation and symptoms caused by thyroid eye disease. There are limited data on teprotumumab's effect on intraocular pressure.
Case presentation:
We report nine patients diagnosed with thyroid eye disease whose intraocular pressure decreased during teprotumumab treatment for 8 weeks: patient 1, a 67-year-old Hispanic woman; patient 2, an 86-year-old African-American man; patient 3, a 71-year-old Caucasian woman; patient 4, a 72-year-old Hispanic woman; patient 5, a 65-year-old Caucasian woman; patient 6, a 54-year-old Caucasian man; patient 7, a 54-year-old Asian man; patient 8, a 31-year-old Asian woman; patient 9, a 60-year-old Caucasian woman. The diagnosis of thyroid eye disease was based on increased redness, swelling, and excessive tearing; abnormal proptosis, lid retraction, and diplopia measurements were also taken during physical examination. Intraocular pressure in primary, lateral gaze, and upgaze was documented. There was significant (p = 0.0397) improvement of primary gaze eye pressure from pre-teprotumumab infusions (baseline) to completion of the treatment course.
Conclusions:
Teprotumumab significantly decreased the intraocular pressure for patients during the duration of the study. Teprotumumab is a novel medication that is approved for the primary treatment of thyroid eye disease in both acute and chronic thyroid eye disease. Previous treatments used to treat thyroid eye disease include glucocorticoids, radiotherapy, or orbital decompression surgery; however, these treatments all have significant limitations. Teprotumumab is an effective noninvasive alternative for decreasing symptoms of thyroid eye disease and, as shown, also lowers intraocular pressure. However, teprotumumab should not be used as a substitute for glaucoma medications; its ability to lower intraocular pressure may be in addition to lowering periorbital pressure and retro-orbital pressure.
Keywords:
Intraocular pressure; Lateral gaze; Primary gaze; Teprotumumab; Thyroid eye disease; Upgaze.
Oxymetazoline hydrochloride ophthalmic solution, 0.1%, boosts the effects of botulinum toxin on blepharospasm: a case series
Aug 05, 2022
Journal of Medical Case Reports volume 16, Article number: 299 (2022)
Abstract
Background:
Oxymetazoline hydrochloride ophthalmic solution (0.1%) is a medication used to treat blepharoptosis. Patients who suffer from blepharoptosis have low-lying eyelids that can hinder their vision. Oxymetazoline hydrochloride ophthalmic solution (0.1%) is prescribed to patients to improve their vision by lifting the upper eyelids. Blepharospasm consists of involuntary, bilateral orbicularis oculi muscle movements that result in twitching and eyelid closure. Botulinum toxin is a treatment used to treat blepharospasm by preventing muscle contraction; but it is not always effective.
Case presentation:
The effects of treatment with both oxymetazoline hydrochloride ophthalmic solution (0.1%) and botulinum toxin are assessed in three patients: (1) Patient A, a 58-year-old Filipina woman; (2) patient B, a 62-year-old Korean woman; and (3) patient C, A 57-year-old Vietnamese woman. All patients had been diagnosed with blepharoptosis as well as blepharospasm. Each patient was given an opportunity to complete an optional survey to assess not only the efficacy of oxymetazoline hydrochloride ophthalmic solution (0.1%) together with botulinum toxin but also their perceived stress during the past month.
Conclusions:
Administering botulinum toxin for the treatment of blepharospasm in patients A and B yielded the expected results; adding oxymetazoline hydrochloride ophthalmic solution (0.1%), a medical treatment for ptosis, to the treatment regimen yielded an unexpected reduction of blepharospasm. We propose that botulinum toxin and oxymetazoline hydrochloride ophthalmic solution (0.1%) can have a synergistic effect on reducing blepharospasm when used concomitantly. We present three cases in which combined use of botulinum toxin with oxymetazoline hydrochloride ophthalmic solution (0.1%) reduced blepharospasm, and propose possible reasons for such effects. We also discuss previous literature in agreement with the results of our cases.
Keywords:
Intraocular pressure; Lateral gaze; Primary gaze; Teprotumumab; Thyroid eye disease; Upgaze.